Estrogen Pills: Risks, Benefits, and Safer Alternatives
Estrogen pills are convenient for hormone therapy but there are serious risks you need to discuss with your doctor
*IV Ketamine, NR, and NAD+ have been used clinically off-label for decades. They are not FDA approved for the treatment of any psychiatric or pain condition. All medical treatments carry risks and benefits that you must discuss with a doctor at Clarus Health to learn if these therapies are right for you.

Estrogen pills: are they safe?
Estrogen pills are a common form of hormone replacement therapy - but oral estrogen pills carry unique risks that patches and creams don't. Here's what every woman should understand before starting them.
Estrogen pills are widely prescribed for menopause and hormone replacement, and for many women, they work well. They're convenient, well-studied, and can meaningfully improve quality of life. But here's the problem: the way a pill is absorbed changes how it behaves in your body - and that difference has real consequences.
What are estrogen pills?
Estrogen pills are oral tablets - most commonly estradiol (identical to what your body makes) or conjugated equine estrogens (CEE, sold as Premarin).
When you take estrogen pills orally, they pass through your gut and get metabolized by your liver before entering your bloodstream - a process called first-pass hepatic metabolism. This is crucial because the liver in turn increases increasing production of certain proteins, including clotting factors. This causes the main risk between estrogen pills and other forms of estrogen.
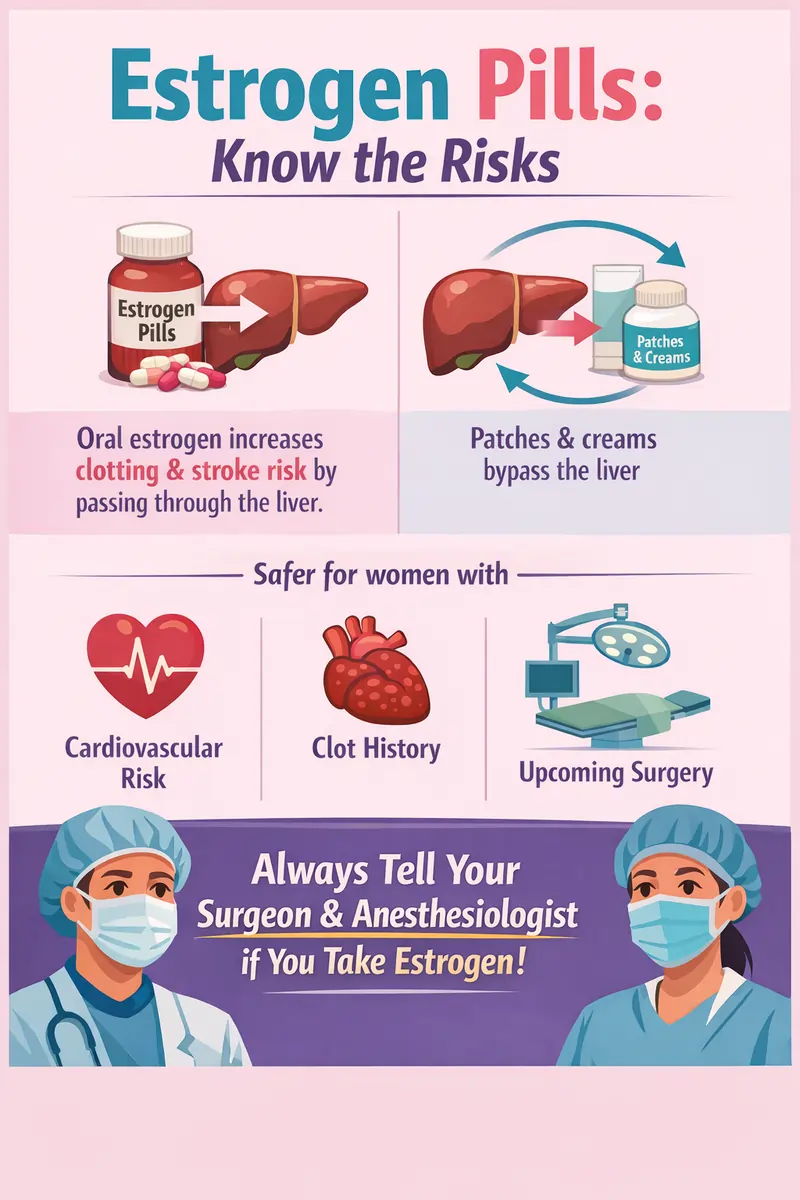
Benefits of estrogen pills
When used in the right patient at the right dose, oral estrogen can be genuinely life-changing. Well-documented benefits include:
- Hot flash and night sweat relief — oral estrogen is highly effective for vasomotor symptoms that disrupt sleep and daily life
- Bone protection — estrogen slows the accelerated bone loss that follows menopause; long-term data from the Women's Health Initiative confirm this protective effect
- Mood and cognitive support — many women report significant improvements in mood, mental clarity, and sleep with estrogen replacement
- Vaginal and urinary health — low estrogen contributes to vaginal dryness, atrophy, and urgency; systemic estrogen can help, though localized vaginal estrogen is often more targeted for these symptoms specifically
- Cardiovascular benefit (when started early) — when initiated within 10 years of menopause onset, estrogen may be cardioprotective; this is sometimes called the "timing hypothesis"
The risks of estrogen pills (the liver matters!)
The liver causes the main difference between estrogen pills, patches, and creams. Because pills are processed by the liver, the liver ramps up production of clotting factors. This mirrors what happens during pregnancy, when rising estrogen levels help prepare the body for the blood loss of childbirth. In that context it's protective. When this happens in non-pregnant woman though, it can be disastrous if it leads to a blood clot or strake.
Transdermal estrogen — patches, gels, and creams — bypasses the liver entirely, which is why multiple large studies show substantially lower blood clot risk with transdermal forms compared to oral.
Blood clot and stroke risk from estrogen pills
Oral estrogen increases the risk of venous thromboembolism (VTE) — clots in the deep veins or lungs — and modestly raises stroke risk in certain populations. This risk varies by dose, formulation, age, and individual clotting history, but it is consistently higher with oral forms than with transdermal alternatives.
Surgery is a high-risk window for estrogen pills
Surgery already elevates clotting risk. Orthopedic procedures like hip and knee replacements add immobilization on top of that. For women on oral estrogen, these two risk factors compound each other. Most guidelines recommend discussing whether to pause or switch oral estrogen before major surgery — but that conversation can only happen if your surgical team knows you're on it.
I want to be direct about something: women are more likely to have hormone-related questions dismissed in clinical settings. It's a real problem my patients face, and it's why some women end up managing HRT on their own — online, or through compounding pharmacies, without telling their other doctors. I understand why that happens. But the cost of that silence can be serious, and your surgeon and anesthesiologist need to know everything going into your body before you go under.
Breast cancer nuance
The relationship between estrogen and breast cancer is highly context-dependent. Estrogen-alone therapy carries a different risk profile than estrogen plus a synthetic progestogen. The type of progestogen also matters — synthetic progestins carry more risk than bioidentical progesterone. Dose, duration, and timing since menopause all factor in. The Women's Health Initiative data is frequently misapplied to all HRT when it applies only to specific types of hormones - this is an area where individualized clinical assessment is not optional.
Estrogen pills vs. patches vs. creams
The hormone matters, but so does how it gets into your body. Here's a comparison:
- Oral pills — convenient and well-studied, but first-pass liver metabolism raises blood clot and stroke risk. Not appropriate for women with a history of blood clots, stroke, significant cardiovascular risk, or genetic risks.
- Transdermal patches — deliver estrogen through the skin, bypassing the liver. Multiple studies show low blood clotting risk. Generally considered the first-line option for women with any cardiovascular risk factors.
- Estrogen creams and gels (skin) — also transdermal, same liver-bypass advantage as patches. Require consistent dosing to be effective. Gels in particular allow for flexible dose titration.
- Vaginal estrogen cream — minimal systemic absorption. Highly effective for vaginal dryness and urinary symptoms specifically, but limited benefit for hot flashes.
For many women, oral estrogen is entirely appropriate. For women with any cardiovascular risk factors, a history of clots, or an upcoming surgery, transdermal is generally the safer starting point.
Getting hormone therapy right: estrogen and beyond
Hormone replacement isn't a one-size prescription. The form of delivery, the type of estrogen and progestogen, the dose, and how it interacts with your other hormones all matter clinically. This is one of the most nuanced areas in medicine, and it's why I don't approach BHRT with a generic protocol.
At Clarus Health, we test over 150 biomarkers and build a hormone protocol around your actual biology, not population averages. If you've had hormone questions brushed off before, or if you're managing this on your own and want to do it safely, I'd encourage you to schedule a free consultation — we can talk through what makes sense for you specifically.




